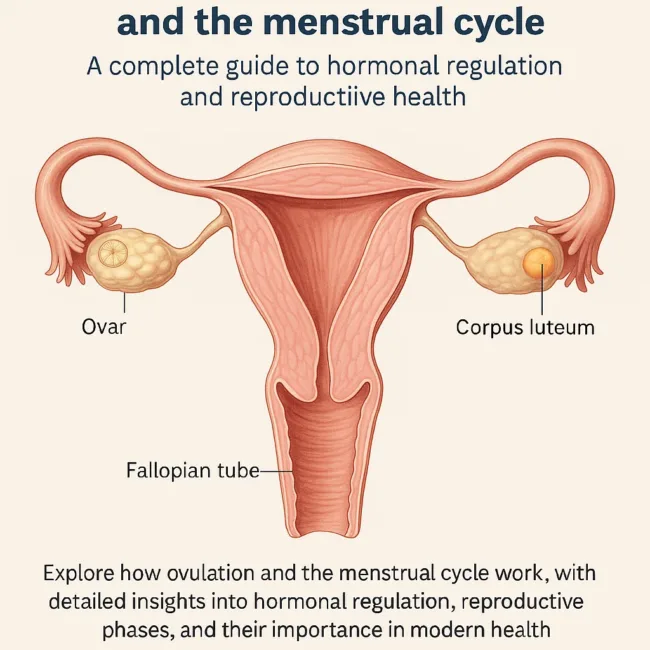
What is the process of ovulation and how does the female reproductive system prepare for it each month?
Ovulation is the cyclical process by which a mature ovum, or egg, is released from an ovarian follicle in preparation for potential fertilization. Unlike sperm production in males, which begins at puberty and continues uninterrupted throughout life, female ova production begins even before birth. By the time a female infant is born, her ovaries already contain thousands of primary oocytes enclosed in follicles. These primary oocytes remain dormant until puberty, at which point hormonal changes initiate their maturation.
At puberty, typically between 13 and 14 years of age, the reproductive system begins functioning in a cyclic pattern. With each menstrual cycle, one ovum matures and is released alternately by each ovary, although the exact timing can vary slightly between women. Ovulation generally occurs once every 28 to 30 days, around the 14th day of a standard cycle. Once released, the ovum remains viable for fertilization for approximately 24 hours. If fertilization does not occur within that period, the ovum degenerates, and the body begins preparing for the next cycle. This process continues monthly until menopause, which generally occurs between 50 and 55 years of age, when the ovaries cease releasing eggs.
How does the menstrual cycle work and why is it important for reproductive and hormonal health in women?
The menstrual cycle is the complex sequence of structural and hormonal changes that prepares the female reproductive system for pregnancy. The cycle, lasting approximately 28 to 30 days, involves the ovaries, uterus, and hormonal signals from the brain. It ensures that the ovum is released at the right time and that the uterine lining is appropriately prepared to receive a fertilized egg. This synchronized process is critical for maintaining reproductive health and is an indicator of normal hormonal balance.
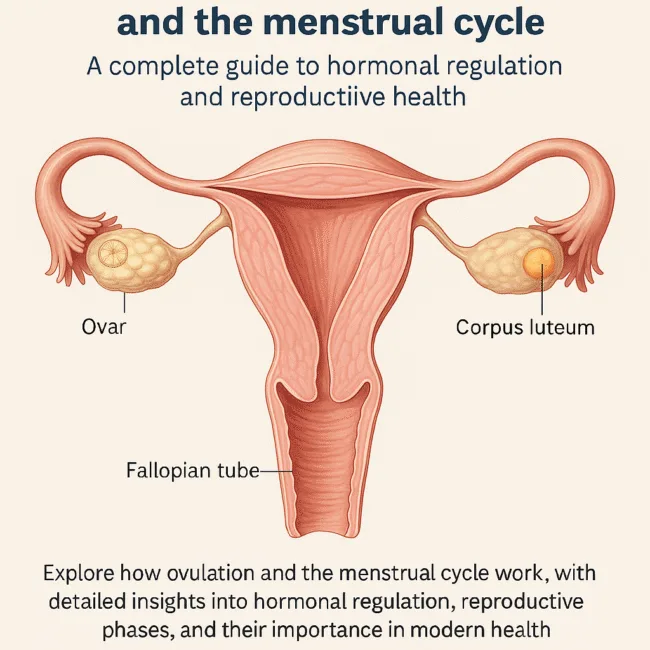
The cycle begins with the first day of menstrual bleeding and is divided into two main phases: the proliferative phase and the secretory phase. These phases involve specific structural changes in the ovaries and uterus, orchestrated by hormones secreted by the pituitary gland and ovaries. In the absence of fertilization, the uterine lining sheds, marking the beginning of a new cycle.
What changes occur in the ovaries and uterus during the proliferative phase of the menstrual cycle?
The proliferative phase marks the first half of the menstrual cycle, beginning on day one and continuing for about 12 to 14 days. This phase is primarily driven by the follicle-stimulating hormone (FSH), secreted by the anterior pituitary gland. Under the influence of FSH, several ovarian follicles begin to grow, but usually only one follicle reaches full maturity.
During this time, repeated mitotic cell divisions occur in the ovarian follicles, uterine lining, fallopian tubes, and vaginal tissues, causing a significant increase in cell number and tissue thickness. The dominant follicle continues to grow and mature, secreting increasing amounts of estrogen, which further stimulates the thickening of the endometrium, or uterine lining. Around the 14th day of the cycle, a surge in luteinizing hormone (LH) triggers ovulation, releasing the mature ovum into the fallopian tube. This phase represents the body’s preparatory stage, where every structural change is designed to optimize the chances of fertilization and successful implantation.
What happens during the secretory phase and how does it prepare the uterus for a potential pregnancy?
The secretory phase is the second half of the menstrual cycle and occurs after ovulation, lasting for approximately 14 to 16 days. Once the ovum is released, the ruptured ovarian follicle transforms into a temporary endocrine structure known as the corpus luteum. The corpus luteum secretes large amounts of progesterone and some estrogen. These hormones stimulate the further thickening and vascularization of the uterine lining, making it nutrient-rich and suitable for the implantation of a fertilized egg.
If fertilization and implantation occur, the developing embryo begins to secrete hormones that maintain the corpus luteum, ensuring continuous progesterone production to support pregnancy. However, if fertilization does not take place, the corpus luteum degenerates by around the 26th day of the cycle. This decline in progesterone and estrogen levels triggers the shedding of the thickened uterine lining along with blood and tissue, resulting in menstrual bleeding. Immediately after this, the proliferative phase begins again, restarting the cycle.
Which hormones control the menstrual cycle and what roles do they play in regulating ovulation and uterine changes?
The menstrual cycle depends on the finely coordinated actions of hormones secreted by the brain and ovaries. The hypothalamus and pituitary gland regulate the release of ovarian hormones through a feedback mechanism. Follicle-stimulating hormone (FSH) is essential for stimulating the growth and maturation of ovarian follicles during the proliferative phase. Luteinizing hormone (LH) triggers the release of the mature ovum and supports the formation of the corpus luteum. Estrogen, secreted by the developing follicles, thickens the uterine lining during the first half of the cycle, while progesterone, secreted mainly by the corpus luteum, maintains the uterine lining during the secretory phase. Prolactin, though mainly associated with milk production after childbirth, plays a minor supportive role in regulating reproductive functions.
The precise timing of hormonal secretion ensures that ovulation occurs only after the uterine lining is adequately prepared for implantation, optimizing the chances of pregnancy. Any disruption in the hormonal balance can lead to irregular cycles, anovulation, or infertility, highlighting the critical importance of hormonal regulation.
Why does the menstrual cycle stop during pregnancy and permanently end after menopause?
When fertilization and implantation occur, the menstrual cycle temporarily halts because the developing embryo produces hormones that signal the corpus luteum to continue secreting progesterone. This prevents the uterine lining from shedding, ensuring a stable environment for pregnancy to continue. This hormonal support is maintained until the placenta fully develops and takes over progesterone production.
Menopause marks the permanent cessation of the menstrual cycle, which usually occurs between the ages of 50 and 55. With age, the ovarian follicles are gradually depleted, and estrogen and progesterone production declines significantly. As a result, ovulation ceases, and the cyclic changes in the ovaries and uterus come to an end.
Why is understanding ovulation and the menstrual cycle important for reproductive health and modern medicine?
Understanding the physiology of ovulation and the menstrual cycle is essential for reproductive health, fertility planning, and diagnosing hormonal or reproductive disorders. Knowledge of the cycle helps in understanding conditions such as polycystic ovary syndrome (PCOS), irregular periods, and early menopause. For medical professionals, this understanding forms the foundation for treatments involving fertility drugs, assisted reproductive techniques, and hormonal therapies.
For health-conscious individuals, tracking the menstrual cycle can provide insights into overall hormonal health, detect early signs of reproductive issues, and assist in planning pregnancy or using contraceptives effectively. Moreover, in modern medicine, the study of hormonal regulation during the menstrual cycle continues to guide innovations in reproductive endocrinology and personalized treatments for infertility.
How does knowledge of ovulation and the menstrual cycle benefit modern health and medicine today?
The menstrual cycle is a reflection of the intricate balance between hormones and reproductive organs, serving as a key indicator of a woman’s overall reproductive and endocrine health. Understanding how the cycle functions is not just important for conception but also for maintaining hormonal balance and diagnosing medical conditions early. Today, this knowledge underpins advances in fertility treatments, hormonal contraceptives, and therapies for menstrual and ovarian disorders, making it as relevant to modern medicine as it is to personal health awareness.
Discover more from Business-News-Today.com
Subscribe to get the latest posts sent to your email.