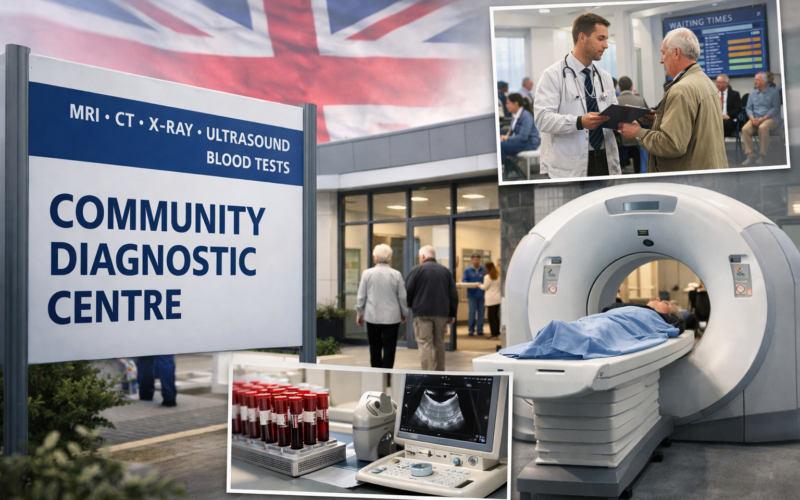
The United Kingdom’s Department of Health and Social Care and NHS England announced on 13 April 2026 a £237 million investment to expand the country’s network of Community Diagnostic Centres across England, adding four new sites and upgrading 32 existing centres in a move designed to accelerate diagnostic capacity and reduce patient waiting times. The announcement is the most significant single tranche of diagnostic infrastructure funding under Health and Social Care Secretary Wes Streeting’s tenure and forms part of the government’s broader £26 billion annual NHS investment programme. The investment directly targets a structural bottleneck in the NHS elective care pathway: diagnostic delays that precede treatment and extend waiting lists. With NHS England having recorded nearly 30 million diagnostic tests in 2025, a new high, the government is signalling that volume expansion alone is insufficient and that geographic redistribution of capacity is equally critical.
How does the £237 million NHS Community Diagnostic Centres investment expand diagnostic capacity across England in 2026?
The funding allocates resources across three tiers of intervention. Four entirely new Community Diagnostic Centres will open during the 2026 to 2027 financial year in Gorton in Manchester, Luton, Boston, and Bideford, each equipped with full imaging and diagnostic suites. A further 17 existing centres will receive physical expansion, meaning new rooms and additional scanning technology including MRI, CT, and ultrasound equipment that will materially increase the volume and range of tests each site can offer. The remaining 15 centres will receive targeted enhancements, adding specialist services such as audiology, ophthalmology, and respiratory care rather than expanding floorspace.
The cumulative effect is that England’s Community Diagnostic Centre network will grow from its current 170 operational sites and will add meaningful capacity at 36 locations. NHS England noted that 108 of the existing centres already operate 12 hours a day, seven days a week, a scheduling model that positions these sites as genuine alternatives to hospital outpatient departments for routine diagnostics.
The strategic logic is straightforward. Community Diagnostic Centres are deliberately sited outside hospitals, in high streets, shopping centres, retail parks, and leisure facilities, making them accessible without the friction of a hospital visit. From a patient behaviour standpoint, this model reduces non-attendance rates and is more amenable to the working population, who might otherwise delay or skip diagnostic appointments that conflict with employment or childcare commitments.
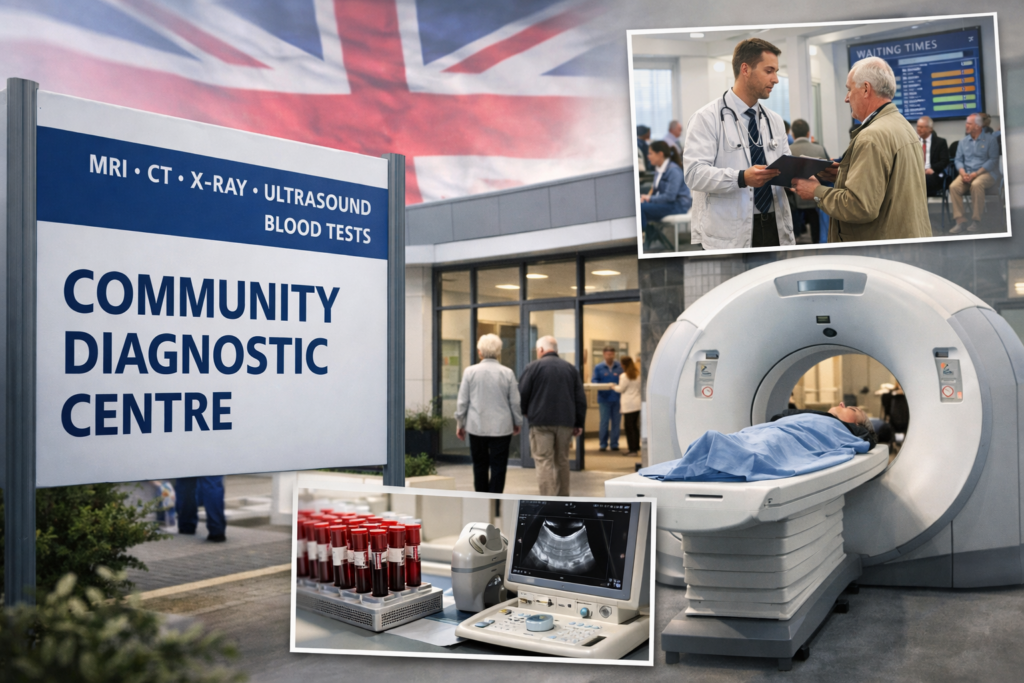
Why the government’s record 29 million NHS diagnostic tests in 2025 does not solve the underlying structural problem
The 29 million figure, which NHS England characterises as a record for diagnostic activity in England, is a genuine operational achievement and reflects the early returns on the CDC programme that began in earnest under the previous government and has been accelerated under the current administration. However, volume metrics do not capture geographic distribution, and high aggregate numbers can mask significant regional variation in access to timely diagnostics.
England’s historical over-reliance on hospital-based diagnostics created a system in which diagnostic capacity was concentrated at large acute trusts, often requiring patients to travel considerable distances and creating additional pressure on hospital site logistics. Shifting diagnostic activity into community settings addresses this structurally rather than operationally, and the government’s decision to fund physical expansion of existing CDCs alongside new openings suggests a deliberate effort to deepen the footprint in areas where capacity is already partially established rather than simply scatter new sites.
The additional 3.5 million tests carried out in the first 18 months of the current government compared to the equivalent prior period is a data point that the Department of Health and Social Care is deploying as evidence of momentum. The more meaningful question for analysts and policymakers is whether the incremental diagnostic volume is generating downstream reductions in the elective waiting list, which at its peak exceeded 7.7 million in England. NHS England has not published equivalent data on treatment waiting times in this announcement, which leaves the causal link between diagnostic expansion and waiting list reduction as an assumption rather than a demonstrated outcome in this specific release.
What the CDC expansion signals about NHS capital investment priorities and the shift toward community-based care
The investment fits within a wider policy trajectory in which NHS England is deliberately attempting to shift activity out of acute hospitals and into primary care, community, and outpatient settings. This is not purely a patient experience initiative; it has significant capital and revenue cost implications. Community diagnostic facilities, particularly those colocated with existing retail or leisure infrastructure, carry lower estate costs than hospital expansions, and the throughput model, characterised by standardised imaging and pathology tests conducted at scale, is well suited to community deployment.
Rory Deighton of The NHS Alliance made the point that a decade of underinvestment in capital has left the health service with outdated buildings and an insufficient stock of modern diagnostic machines. This is a substantive observation. NHS England’s diagnostic estate is not uniformly modern, and the centres receiving targeted enhancements under this funding round reflect sites where equipment or service gaps exist within an otherwise functional CDC framework.
The pathology dimension of this expansion, highlighted by the Royal College of Pathologists, deserves attention. Pathology services including blood testing, monitoring of chronic conditions such as heart disease, diabetes, and kidney function, and early cancer screening underpin a significant proportion of diagnostic activity and are integral to the CDC operating model. The integration of pathology into community settings is a material step toward earlier diagnosis of conditions that are currently identified too late for optimal treatment outcomes, which has both clinical and health economic implications.
How does the NHS Community Diagnostic Centres model reduce pressure on hospital outpatient departments and elective waiting lists?
The mechanism is straightforward in theory. By conducting MRI, CT, ultrasound, blood tests, and a range of specialist assessments at community sites, NHS England reduces the volume of patient journeys that would otherwise terminate at hospital outpatient departments. This has two compounding effects: it frees outpatient appointment slots for cases that genuinely require hospital-level clinical expertise, and it reduces the referral-to-diagnosis timeline for patients whose diagnostic need is relatively routine but who would otherwise sit in a queue behind more complex cases.
The addition of audiology, ophthalmology, and respiratory care services at enhanced CDCs extends this logic into specialties where community-based assessment is clinically appropriate and where hospital waiting lists have historically been long. Ophthalmology in particular has been a persistent pressure point in NHS outpatient activity, and shifting a proportion of screening and assessment capacity into CDCs is a measured response to that backlog.
The execution risk in this model sits at the workforce layer. Community diagnostic services require trained radiographers, sonographers, pathologists, and specialist nurses, and NHS England faces known shortages across several of these groups. Adding physical capacity and equipment without a parallel workforce plan creates the risk of underutilised sites, a pattern that has appeared in previous NHS capital programmes. This announcement does not include specific commitments on workforce expansion, which is a gap that will need to be addressed for the investment to deliver its intended throughput gains.
Key takeaways on what the £237 million NHS Community Diagnostic Centres expansion means for healthcare delivery, NHS policy, and the elective care agenda
- The government’s £237 million investment expands England’s CDC network to more than 170 operational sites, with four new centres opening in 2026 to 2027 and 32 existing sites receiving physical or equipment upgrades.
- The CDC model is a deliberate structural response to the over-concentration of diagnostic capacity in acute hospital settings, addressing both geographic access gaps and hospital operational pressure simultaneously.
- NHS England’s record 29 million diagnostic tests in 2025 validates the programme’s volume trajectory but does not, in isolation, confirm that diagnostic expansion is translating into proportional reductions in the elective waiting list.
- The integration of audiology, ophthalmology, respiratory, and pathology services into CDCs broadens the programme’s clinical scope beyond standard imaging and increases the relevance of community diagnostics to chronic disease management and early cancer detection.
- Workforce availability, specifically trained radiographers, sonographers, and specialist nurses, remains the primary execution risk and is not directly addressed in this funding announcement.
- The 12-hour, seven-day operating model deployed across 108 existing CDCs is structurally aligned with working-age population access needs and is likely to produce better attendance compliance than traditional outpatient appointment scheduling.
- The £237 million commitment sits within a £26 billion annual NHS investment envelope, positioning diagnostic infrastructure as a capital priority within the government’s broader NHS recovery agenda.
- Community diagnostic infrastructure built within retail and leisure settings represents a lower-cost estate model than hospital expansion and is better suited to standardised, high-volume testing workflows.
- The expansion has clear health inequality implications, with new sites in Gorton, Luton, Boston, and Bideford serving populations that may have faced greater diagnostic access barriers than those in urban centres with established NHS infrastructure.
- Second-order beneficiaries include medical imaging equipment manufacturers and suppliers, private diagnostic service operators contracted to run CDC sites, and NHS workforce training providers, all of whom stand to see increased demand as the programme scales.
Discover more from Business-News-Today.com
Subscribe to get the latest posts sent to your email.